Retrocalcaneal Bursitis Treatment for Heel Bone Pain
Photo from Unsplash
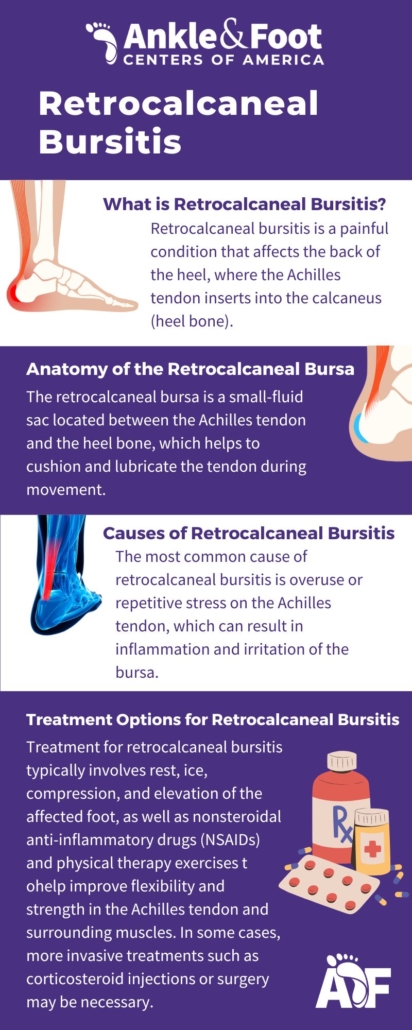
What is Retrocalcaneal Bursitis?
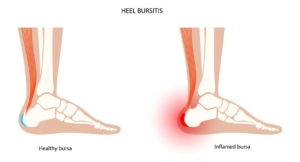
Retrocalcaneal bursitis is a condition characterized by the inflammation of the bursa located at the back of the heel. The bursa acts as a cushion between the heel bone and the Achilles tendon, which connects the calf muscle to the heel bone. When the bursa becomes inflamed, it can cause pain, swelling, and stiffness in the back of the heel, making it difficult to walk, run, or wear certain types of shoes.
The most common causes of bursitis in the heel include overuse or repetitive strain, trauma to the back of the heel, abnormal foot mechanics, and medical conditions such as rheumatoid arthritis. Symptoms of retrocalcaneal bursitis may include pain and tenderness at the back of the heel, swelling and redness, stiffness, and difficulty walking or running.
Importance of Diagnosing and Treating Heel Bursitis Early
Early diagnosis and treatment of retrocalcaneal bursitis are crucial to managing symptoms and preventing the condition from worsening. Ignoring the symptoms or delaying treatment can lead to chronic pain and further damage to the Achilles tendon. Seeking medical attention at the first sign of symptoms can help identify the underlying cause and determine the best course of treatment to relieve pain and restore normal function to the foot and ankle.
Causes of Retrocalcaneal Bursitis
Retrocalcaneal bursitis can be caused by a variety of factors, including overuse or repetitive strain, trauma to the back of the heel, abnormal foot mechanics, and medical conditions such as rheumatoid arthritis. Identifying the underlying cause of retrocalcaneal bursitis is crucial to managing symptoms and preventing the condition from worsening.
- Heel Bursitis From Overuse or Repetitive Strain – Overuse or repetitive strain on the bursa can cause retrocalcaneal bursitis, particularly in individuals who engage in activities that involve frequent and forceful heel strikes. Runners, dancers, and athletes who participate in jumping sports are at increased risk of developing retrocalcaneal bursitis due to the repetitive nature of these activities.
- Heel Trauma – Direct trauma to the back of the heel can cause retrocalcaneal bursitis. This may occur due to a fall, a blow to the heel, or wearing poorly fitting shoes that place excessive pressure on the bursa.
- Abnormal foot mechanics – Abnormal foot mechanics, such as flat feet or high arches, can place extra stress on the bursa and increase the risk of developing retrocalcaneal bursitis. Individuals with abnormal foot mechanics may require orthotic devices to help redistribute pressure on the bursa and prevent further inflammation.
- Medical conditions – Certain medical conditions, such as rheumatoid arthritis, gout, and infection, can cause inflammation of the bursa and lead to retrocalcaneal bursitis. Managing these underlying medical conditions is essential to preventing the development or recurrence of retrocalcaneal bursitis.
If you suspect you have retrocalcaneal bursitis, it is important to seek medical attention to receive a proper diagnosis and determine the best course of treatment to manage your symptoms and prevent further complications.
Symptoms of Retrocalcaneal Bursitis
Symptoms of retrocalcaneal bursitis may include pain and tenderness at the back of the heel, swelling and redness, stiffness, and difficulty walking or running. If left untreated, symptoms may worsen over time and lead to further complications, such as Achilles tendonitis or a ruptured Achilles tendon.
- Pain and Tenderness at the Back of the Heel – The most common symptom of retrocalcaneal bursitis is pain and tenderness at the back of the heel, particularly when pressure is applied to the area. This pain may be sharp or dull and can range from mild to severe.
- Swelling and Redness – Inflammation of the bursa can cause swelling and redness at the back of the heel, which may make it difficult to wear certain types of shoes or engage in activities that involve repetitive heel strikes.
- Stiffness – Stiffness in the ankle and difficulty moving the foot up and down may also be symptoms of retrocalcaneal bursitis. This stiffness may be particularly noticeable in the morning or after prolonged periods of inactivity.
- Difficulty walking or running – As the condition worsens, individuals with retrocalcaneal bursitis may experience difficulty walking or running due to pain and stiffness in the ankle and heel.
Diagnosis of Retrocalcaneal Bursitis
Diagnosing retrocalcaneal bursitis typically involves a physical examination, patient history, and imaging tests to confirm the diagnosis and rule out other conditions that may cause similar symptoms.
Physical Examination and Patient History
During a physical examination, a local podiatrist will look for signs of inflammation and tenderness at the back of the heel. They may also ask about your medical history, including any previous injuries or medical conditions that may increase your risk of developing retrocalcaneal bursitis.
X-rays and Other Imaging Tests
Imaging tests, such as X-rays or ultrasound, may be used to confirm the diagnosis of retrocalcaneal bursitis and rule out other conditions that may cause similar symptoms, such as a stress fracture or tendonitis.
MRI scan
In some cases, an MRI scan may be ordered to provide a more detailed image of the bursa and surrounding tissues, which can help with the diagnosis and treatment plan.
If you suspect you have retrocalcaneal bursitis, it is important to seek medical attention to receive a proper diagnosis and determine the best course of treatment to manage your symptoms and prevent further complications. Early diagnosis and treatment are crucial to preventing chronic pain and long-term damage to the Achilles tendon.
Treatment Options for Retrocalcaneal Bursitis
 There are several treatment options available for retrocalcaneal bursitis, including rest and ice, non-steroidal anti-inflammatory drugs (NSAIDs), physical therapy, heel lifts and orthotic devices, corticosteroid injections, extracorporeal shock wave therapy (ESWT), and surgery. The appropriate treatment will depend on the severity of the symptoms and the underlying cause of the condition.
There are several treatment options available for retrocalcaneal bursitis, including rest and ice, non-steroidal anti-inflammatory drugs (NSAIDs), physical therapy, heel lifts and orthotic devices, corticosteroid injections, extracorporeal shock wave therapy (ESWT), and surgery. The appropriate treatment will depend on the severity of the symptoms and the underlying cause of the condition.
Rest and Ice
Resting the affected foot and applying ice to the affected area can help reduce inflammation and pain. In some cases, a walking boot or crutches may be recommended to help take pressure off the bursa and promote healing.
Non-Steroidal Anti-Inflammatory Drugs (NSAIDs)
Over-the-counter or prescription NSAIDs, such as ibuprofen or naproxen, can help relieve pain and reduce inflammation. It is important to talk to your doctor before taking any medications to ensure they are safe for you and do not interact with any other medications you are taking.
Physical Therapy
Physical therapy can help strengthen the muscles in the foot and ankle, improve range of motion, and promote healing. This may involve exercises, stretches, or other treatments, such as ultrasound or electrical stimulation.
Heel Lifts and Orthotic Devices
Heel lifts or orthotic devices can help redistribute pressure on the bursa and reduce inflammation. These devices are typically customized to fit the individual’s foot and address any abnormal foot mechanics that may be contributing to the condition.
Corticosteroid Injections
Corticosteroid injections can help reduce inflammation and pain in the affected area. These injections are typically performed under ultrasound guidance and may be repeated if necessary.
Extracorporeal Shock Wave Therapy (ESWT)
ESWT involves using high-frequency sound waves to promote healing and reduce inflammation. This treatment is typically reserved for individuals who have not responded to other treatments.
Surgery
In severe cases of retrocalcaneal bursitis, surgery may be necessary to remove the inflamed bursa and reduce pressure on the Achilles tendon.
Heel Injections for Retrocalcaneal Bursitis
Heel injections, such as corticosteroid injections or platelet-rich plasma (PRP) injections, can be an effective treatment option for retrocalcaneal bursitis in individuals who have not responded to other treatments.
Types of heel injections:
There are two main types of heel injections used to treat retrocalcaneal bursitis: corticosteroid injections and platelet-rich plasma (PRP) injections.
- Corticosteroid Injections – Corticosteroid injections involve injecting a powerful anti-inflammatory medication into the affected area to reduce inflammation and relieve pain. This treatment is typically performed under ultrasound guidance and can be repeated if necessary.
- Platelet-rich Plasma (PRP) Injections – PRP injections involve using the patient’s own blood to create a concentrated solution of platelets, which are then injected into the affected area to promote healing and reduce inflammation.
Effectiveness of heel injections
Heel injections can be an effective treatment option for retrocalcaneal bursitis in individuals who have not responded to other treatments. Studies have shown that heel injections can provide significant pain relief and improve function in individuals with retrocalcaneal bursitis.
Risks and side effects of heel injections
Heel injections are generally safe and well-tolerated, but there are some risks and potential side effects, such as infection, bleeding, nerve damage, or a temporary increase in pain. Your doctor will discuss the potential risks and benefits of heel injections with you before recommending this treatment option.
Prevention of Retrocalcaneal Bursitis
While it may not always be possible to prevent retrocalcaneal bursitis, there are several measures individuals can take to reduce their risk of developing the condition.
Wear Proper Footwear
Wearing proper footwear with good arch support and cushioning can help reduce stress on the bursa and prevent overuse injuries. Avoid wearing shoes that are too tight or too loose, and make sure they fit well and provide adequate support.
Gradual Increase in Physical Activity
Gradually increasing physical activity, such as running or jumping, can help reduce the risk of overuse injuries that can lead to retrocalcaneal bursitis. It is important to allow adequate rest between activities and not to push yourself too hard too quickly.
Stretching and Strengthening Exercises
Stretching and strengthening exercises can help improve flexibility and strength in the foot and ankle, reducing the risk of injuries and promoting healing. A physical therapist can recommend exercises tailored to an individual’s needs and goals.
If you have a medical condition that increases your risk of developing retrocalcaneal bursitis, such as rheumatoid arthritis, it is important to work with your healthcare provider to manage the condition and reduce your risk of complications. By taking these preventative measures, individuals can reduce their risk of developing retrocalcaneal bursitis and maintain healthy foot and ankle function.
